 Click here for a print-ready PDF of this page. Read other articles in the Essential Elements series here. |
Medicaid Overview
Medicaid is a joint federal-state program that funds health care services on a means-tested basis for eligible low-income Americans. Although states must operate within certain federal requirements, each state sets its own Medicaid regulations and provider reimbursement rates, and decides who qualifies for benefits and what benefits to provide. This program is different than Medicare, a federally run program that covers seniors and certain people with disabilities in the U.S.
Medicaid typically provides a comprehensive set of health care services, although access to care may be a challenge in some areas where not enough health care providers accept Medicaid patients. Out-of-pocket costs for Medicaid beneficiaries are low, with no or very low premiums or copayments. States may operate Medicaid programs in which health care providers directly bill the state agency or may utilize managed care organizations (MCOs) that coordinate a beneficiary’s health care needs.
Medicaid Population
States have the option to extend coverage beyond the above populations to individuals who have higher income levels than the federal minimums.
The Affordable Care Act (ACA) provided an option for states to expand Medicaid coverage, targeting non-elderly (primarily childless) adults with incomes at or below 138 percent of the federal poverty level (FPL).1 The expansion provides health insurance to non-elderly adults with incomes above states’ limited eligibility levels, thus reducing the level of those uninsured, both at the state and national level. Due to a June 2012 ruling by the U.S. Supreme Court, Medicaid expansion is optional for states, rather than mandatory as originally provided for in the ACA. Currently 27 states plus the District of Columbia have opted for expansion, and two states have not made a decision regarding expansion.
|
MEDICAID SERVICES
|
Dual Eligibles
Dual eligibles refer to individuals (older Americans and younger individuals with disabilities) who qualify for both Medicare and some level of Medicaid services. There are currently approximately 9.6 million dual eligibles. Medicare is the primary payer for dual eligibles, with Medicaid covering certain gaps in coverage not provided by Medicare (e.g., payment of Medicare premiums, deductibles, and cost-sharing). Dual eligible often are some of the poorest, least healthy individuals in the Medicare and Medicaid programs.
Medicaid Coverage
Medicaid mandatorily covers an array of services which include, but are not limited to: physician services, inpatient and outpatient hospital services, long-term care services and supports, laboratory and X-ray services, and family planning services. Almost all states cover services that are deemed optional (not mandated) by the federal government, including prescription drugs, and preventive, rehabilitative, and hospice care. In states opting for expansion under the ACA, newly eligible adults covered by Medicaid will receive Alternative Benefits Plans that may or may not match Medicaid program benefits, but which are required to include all 10 essential health benefits that are offered in the exchanges.2
Over half of Medicaid beneficiaries receive care through Medicaid MCOs that contract with states and receive per-beneficiary payments to administer Medicaid services. In addition, a smaller share of Medicaid beneficiaries receive care through Primary Care Case Management (PCCM) programs, in which states continue to pay providers fee-for-service while also paying primary care providers a small monthly fee for care coordination. Regular fee-for-service reimbursement constitutes the remainder of Medicaid provider payments.
Current Status of State Medicaid Expansion Decisions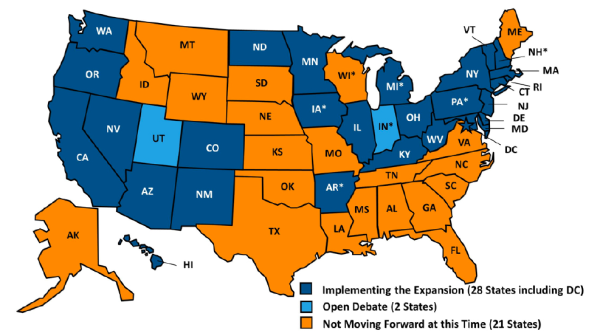 Source: “Current Status of State Medicaid Expansion.” Kaiser Family Foundation (Aug. 28, 2014). Based on data from the Centers for Medicare and Medicaid Services.
|
Medicaid Financing
Medicaid’s spending has been growing faster than the overall U.S. economy, and the program’s spending is expected to increase on average about 6.8 percent annually from 2015 through 2023, according to the Centers for Medicare & Medicaid Services (CMS). The state Medicaid share and public school education typically comprise the largest expenses of state budgets, and Medicaid’s growing costs continue to be a matter of intense concern during state fiscal deliberations between governors and legislatures. According to CMS, combined federal and state Medicaid spending is estimated to be over $900 billion in 2023 (double from 2013) for expected coverage of over 80 million Americans. Whereas Medicaid was approximately 1 percent of gross domestic product (GDP) in 1985, it could approach 3.4 percent of GDP in 2023.
The federal share for Medicaid – which varies by state based on a formula – ranges from 50 percent to almost 74 percent for 2015. A higher medical assistance percentage is provided to states with lower per capita income. For certain benefits or populations, states may receive federal matching funds at a higher percentage than through the formula calculation.
As provided under the ACA, the federal government will fund 100 percent of the cost for Medicaid expansion beneficiaries in those states that opted for it through 2016; that share will decline gradually to 90 percent by 2020 and beyond.
Long-term Care
Medicaid, which is the nation’s largest funder of long-term care services, has historically been heavily programmed toward institutional care for long-term care services. But through changes provided in ACA, states have been given additional flexibility and federal funds to provide services inhome, and through senior centers and other community groups. Additionally, a dozen states are testing models to better integrate and coordinate long-term care services and supports between Medicare and Medicaid for dual eligibles.
The Long-Term Care Partnership Program is a joint state public-private program to incentivize individuals to purchase private long-term care insurance in order to help them pay for long-term care services. Provided for by a 2005 federal law3 that expanded the partnerships beyond limited state pilot programs, the purchase of the coverage was regarded as a benefit to both the policyholder and the public in order to help eliminate, reduce, or delay the need for those individuals to access Medicaid long-term care coverage, which has often been done by a Medicaid “spend-down” where assets have to be spent before Medicaid covers long-term care services.
Conclusion
The Medicaid program is vital to the health of millions of low-income Americans, including children, adults, seniors, and persons with disabilities. States are given flexibility to tailor their Medicaid programs, within certain parameters, to their own unique needs and circumstances. The ACA has added a considerable expansion of Medicaid eligibility to a broader population, including basic, essential benefits plans for newly eligible adults. The growing cost of the Medicaid program remains an ongoing fiscal challenge for both state and federal governments, even with the federal government funding most of Medicaid expansion populations going forward.
Footnotes
1. http://aspe.hhs.gov/poverty/14poverty.cfm
2. As defined in section 1302(a) of the Patient Protection and Affordable Care Act. http://www.gpo.gov/fdsys/pkg/PLAW-111publ148/pdf/PLAW-111publ148.pdf
3. The Deficit Reduction Act of 2005 created the Qualified State Long Term Care Partnership program.
 1850 M Street NW • Suite 300 • Washington, DC 20036 • 202.223.8196 Copyright 2014 American Academy of Actuaries. All rights reserved |







